Jeffrey C. Riley Commissioner
June 25, 2020
Opening Letter from Commissioner Jeffrey C. Riley
June 25, 2020
Dear Fellow Educators, School Administrators, Parents, and Community Members,
After a spring unlike any before, I write to you about our plans for the fall with the wellbeing of our students, teachers, staff, and communities firmly in mind. It is sobering to think of the sickness and fatalities caused by COVID-19 in our state, in our nation, and around the world. It is also distressing to witness the murder of George Floyd and others and know that this is a reflection not of a single incident, but a long history of inequity. Through the lens of these two issues, we look at how to best open our schools this fall.
After weeks of discussion with many stakeholders, including our members of our Return-to-School Working Group, infectious disease physicians, pediatricians, and other public health experts; a thorough review of the medical literature; and evaluating what works best for our students, we want to start the school year with as many of our students as possible returning to in-person settings—safely. If the current positive public health metrics hold, we believe that when we follow critical health requirements, we can safely return to in-person school this fall with plans in place to protect all members of our educational community.
Part of our responsibility as educators, administrators, and parents is to do all that we can to help our children in this difficult time. As we all know, there is no substitute for the attention and engagement that is only possible with in-person learning. We can mitigate the risks associated with COVID-19 for in-person school programs and prevent the significant consequences of keeping students out of school and isolated. It will take all of us working together to make this successful.
In the memo that follows, DESE is providing initial guidance for school reopening this fall that prioritizes getting our students back to school in person—safely, following a comprehensive set of health and safety requirements. At the same time, DESE is requiring each district and school to also plan for remote learning and a hybrid school model, a combination of in-person and remote learning, should local conditions change this fall or winter.
The fall reopening guidance comes from a place of deep care and concern, with a focus on translating the public health data and evidence into practical application for school settings. We also acknowledge that it will likely elicit many new questions. We intend to address the most common questions in a running series of FAQs, along with additional specific topical guidance throughout the summer.
I look forward to hearing from you and working together to plan for our children’s individual and collective success in the school year ahead.
Jeffrey C. Riley
Commissioner of Elementary and Secondary Education
MEMORANDUM
To: Superintendents, Charter School Leaders, Assistant Superintendents, Leaders of Special
Education Schools, and Collaborative Leaders
Fr: Jeffrey C. Riley, Commissioner
Date: June 25, 2020
Re: DESE Initial Fall School Reopening Memo
With this memo, we are providing districts and schools with initial guidance on reopening for the fall. In this guidance, we:
· Clearly state our goal for this fall: the safe return of as many students as possible to in-person school settings, to maximize learning and address our students’ holistic needs. If the current positive public health metrics hold, we believe that by following critical health requirements, we can safely return to in-person school.
· Provide a clear set of health and safety requirements for in-person learning this fall, grounded in the most up-to-date scientific literature and discussions with expert medical advisors. While subject to revision as the COVID-19 pandemic evolves and more scientific evidence becomes available, these requirements will serve as an initial planning blueprint for the in-person return of students and staff this fall.
· Require districts and schools to prepare a reopening plan that addresses three possible learning models for this fall: in-person learning with new safety requirements, a hybrid of in-person and remote learning, and the continuation of remote learning (to ensure continuity of learning throughout the school year, even if circumstances change). Schools will also need a focused plan for special student populations. Districts and schools will be required to submit a comprehensive reopening plan to the Department of Elementary and Secondary Education (DESE) in August that addresses these three models. More information will follow shortly.
· Outline the future guidance and other supports that DESE will provide in the coming weeks.
This initial fall memo is one of several updates you will receive from us about fall reopening, with more information to come in July. Districts and schools have already received initial supplies guidance and also two documents for summer school planning – initial summer school guidance and guidance on summer 2020 special education services. Earlier this spring, we also provided initial and then more comprehensive guidance on remote learning.
Developing this initial fall memo required us to draw on the perspectives of both the educational and medical communities. To that end, this guidance reflects weeks of intensive conversations with education stakeholders, including our Return-to-School Working Group, and collaboration with infectious disease physicians, pediatricians and public health experts from the Massachusetts General Brigham Health System and the Massachusetts chapter of American Academy of Pediatrics. Our process has included a close review of guidelines from the Centers for Disease Control (CDC) and World Health Organization (WHO), as well as available medical literature on COVID-19 related to children and school settings. Finally, we consulted with the MA COVID-19 Command Center’s Medical Advisory Board, comprised of physicians and other health experts, which carefully reviewed the health and safety requirements for in-person learning outlined in this document.
Background and context
On March 17, 2020, all elementary and secondary public and private schools in the Commonwealth were ordered to cease in-person instruction, as part of the statewide plan to combat the COVID-19 pandemic and rapidly reduce the transmission of the novel coronavirus. This closure was later extended to last through the end of the 2019-20 school year.
We are currently in Phase 2 of Reopening Massachusetts, and more businesses are able to resume operations with restrictions and capacity limitations. We are optimistic that with our collective continued vigilance (wearing masks, hand washing/sanitizing, staying home when sick), Massachusetts will continue to progress through subsequent reopening phases.
The virus has had different impacts on communities across the state; several cities and towns were impacted significantly, while others have had few infections and no reported fatalities. Over the past several weeks, Massachusetts has seen rates of infections, hospitalizations and fatalities fall steadily, even as the virus remains a significant concern in several communities. As we all know, the COVID-19 context in Massachusetts is not static, and we will continue to monitor the situation closely.
At the same time, other countries have taken steps to reopen schools, which has provided the medical community with an opportunity to study the impacts of the virus in school settings and on children, providing valuable data and strategies that have been effective in reducing the risk of infection and transmission.
In our discussions with infectious disease physicians and other health experts, we have used both local and international data, trends, and case studies to inform our initial guidance for the fall.
Our goal for this fall
Our goal for the fall is to safely bring back as many students as possible to in-person school settings, to maximize learning and address our students’ holistic needs. With the information provided in this memo, districts and schools should begin planning for a fall return that includes multiple possibilities, with a focus first and foremost on getting our students back into school buildings.
There is a clear consensus from both education and medical groups: we must keep in mind not only the risks associated with COVID-19 for in-person school programs, but also the known challenges and consequences of keeping students out of school. While remote learning has improved over the course of the school closures, there is no substitute for in-person instruction when it comes to the quality of students’ academic learning. In-person school plays an equally important role in our ability to support students’ social-emotional needs, including their mental and physical health, and in mitigating the impacts of trauma. We also recognize how disruptive school closures have been to families trying to maintain regular work schedules and manage household needs, including childcare, while also facilitating remote learning.
Moreover, in light of recent events and a national movement to fight for racial justice, it is even more critical that our students are able to quickly return to robust learning opportunities and a supportive school environment, through which we can engage in meaningful discussions on anti-racism, provide mental health supports, and help to prepare our young people to bring about the changes our world desperately needs.
In discussions with infectious disease physicians, other medical advisers, and the COVID-19 Command Center’s Medical Advisory Board, we were heartened to learn that – based on current data and research – the medical community supports the return of our students to in-person learning, with appropriate health and safety guardrails in place. With adherence to a comprehensive set of critical health and safety requirements, we can bring our students, staff, and families safely back to school.
Most of us are now quite familiar with the critical health and safety practices that reduce the risk of transmission of COVID-19. These include rigorous hygiene and handwashing, use of masks/face coverings, physical distancing, reducing interaction between groups, staying home when sick, protecting those most vulnerable to the disease, and expanding testing and tracing capabilities, among others.
However, what can often get lost in long lists of practices is that it is not one mitigation strategy, but a combination of all these strategies taken together that will substantially reduce the risk of transmission. In other words, establishing a culture of health and safety in our schools that focuses on regularly enforcing these important practices is more important than any one measure.
Contextual factors
We recognize that several critical factors affect our ability to bring students back to in-person school settings this fall.
Financial resources. For planning purposes, districts and schools should assume a “level service plus” budget in order to bring students back in person; in other words, additional funds on top of their projected budgets to manage additional costs associated with health and safety preparations. We also recognize that “level service plus” must include additional resources targeted to our historically under-resourced communities. While schools and districts, through the city or town in which they are located, have already received federal CARES Act funds to support COVID-19 related purchases such as health and safety supplies/PPE, technology, and facilities upgrades, the Commonwealth is making additional funding sources available directly to schools and districts to support reopening.
To date, the following federal grants have been available to cities and towns for educational expenses related to COVID-19:
· $193.8 million from the Elementary and Secondary School Emergency Relief (ESSER) Fund to districts, largely based on the Title I formula.
· A portion of the $502 million from the Coronavirus Relief Fund (CvRF) already allocated to cities and towns, of which a meaningful amount of submitted costs are related to education.
· Up to $15 million in competitive federal funds for which the Executive Office of Education (EOE) and DESE have applied.
In addition to the above funds, the Commonwealth is making available:
· An additional $202 million from the CvRF for a new grant round to support school reopening. Of the $202 million, $182 million will be formula grants ($225 per pupil) and $20 million will be available at the Commissioner’s discretion for distribution to districts with unmet needs. In accordance with federal rules, these funds must be spent by December 30, 2020 for COVID-19 related expenses. Funding for the City of Boston and Plymouth County are separate and in addition to these funds.
· $25 million available for remote learning technology grants through which the Commonwealth will provide a 100% state match to districts for their remote learning needs.
While school and district budgets remain uncertain, these additional resources will support schools and districts to provide a healthy and safe environment for in-person learning in the fall.
Cold/flu season. Flu season is another critical factor that could pose significant challenges for schools and students. Not only do flu symptoms closely mirror COVID-19 symptoms, but managing both a bad flu season and ongoing presence of COVID-19 could be highly disruptive for our educational institutions and healthcare system. It is essential that the educational and public health communities, as well as cities and towns, work closely together to ensure as many children and adults as possible receive flu vaccines this fall. Given the high priority of flu vaccinations, particularly this year, the administration will work with these key stakeholders and others on a strategy to enhance flu vaccination coverage in Massachusetts, particularly among school aged children. More guidance will be coming from the Department of Public Health.
Trajectory of COVID-19. All guidance in this document is based on the best information we have as of mid-June. We will carefully monitor the data in the coming weeks and months. Districts and schools must be prepared to be flexible and ready to pivot if circumstances change significantly. For this reason, districts and schools must plan not only for in-person learning, but also hybrid learning models (in which students learn in-person for some of the time and remotely for some of the time), and also full remote learning. Remote learning may be a necessary option in the fall for some students who are unable to return to school due to underlying medical conditions and potentially for all students if COVID-19 forces widespread school closures in the future.
Supporting educators and staff
Our educators and staff are essential to our success as a Commonwealth in preparing for a safe and successful fall reopening. We recognize that educators have been concerned about the challenges of remote learning and student learning loss during school closures this spring, and many educators have been balancing their teaching duties with their own family and personal needs. Some have felt the devastating impact of the virus personally.
We also know educators are eager to teach their students in person again, and that staff members are concerned about the health and safety of their students as well as their own health and safety. We are committed to supporting you with guidance and training as we prepare for fall reopening.
Based on the combination of health and safety requirements and rigorous protocols that we are putting in place for the fall, we believe the risk of transmission in schools is likely lower than the risk of transmission in many other settings. Furthermore, based on available data and effective implementation of critical health and safety practices, the rate of in-school transmissions has been low.[1] [2] [3] [4]
We recognize that planning for reopening in this “new normal” will not be easy; we also know that planning is not nearly as important – nor as difficult – as execution. To have a successful school year, we will all have to be problem-solvers, flexible and responsive to data, and willing to course-correct as necessary. It is also important to acknowledge that there will be COVID-19 positive cases in schools, and we will have protocols to help you determine the appropriate next steps when this happens to keep the school community safe.
Educators and other staff who are at higher risk of severe illness from COVID-19 will want to consult with their health care providers about whether and under what circumstances a return to in-person school settings would be medically inadvisable. We will provide guidance to support districts in working with their educators and staff on critical reopening issues, including those who are at higher risk of severe illness from COVID-19.
Recognizing the special role of families
Families, in consultation with their medical providers, will ultimately make the decision as to whether their children will attend in-person instruction, or whether their children will continue with remote learning. Districts should engage regularly and substantively with families in their primary language to ensure that they have accurate and up-to-date information to make informed decisions about whether an in-person return is best for their children. This also means that all districts will need to have a remote learning program in place for students who are unable to return to in-person school.
Families also play a critical role in supporting the new culture of health and safety that each school must establish. Most importantly, families can help mitigate the transmission of COVID-19 in their school communities by checking their children daily for any COVID-19 symptoms and keeping them home from school if they are sick or have had close contact with a person diagnosed with COVID-19. Families can also contribute by supporting the use of masks in school and on the bus, arranging alternate transportation whenever possible, communicating with teachers, school leaders and local authorities, and continuing to follow state guidance on health and safety outside of school. DESE will provide further guidance and resources for families.
Emerging implications from the medical literature
This section summarizes some of the emerging themes and implications from the medical literature on childhood susceptibility to and transmission of COVID-19 as of mid-June 2020. Because COVID-19 is a novel disease, this literature is growing rapidly, and new information is emerging almost every day. Our guidance will continue to evolve as the science develops.
At this time, the evidence suggests schools have not played a significant role in COVID-19 transmission and that children, particularly younger children, are less likely than adults to be infected with COVID-19. Furthermore, if they become infected, it appears children may be less likely to transmit COVID-19 to others. Based on these initial findings, the health and safety requirements throughout this guidance, as well as considering the key features of school programming at different grade spans, the current evidence supports a safe in-person return to school with implementation details varying for elementary schools (including pre-kindergarten programs), middle schools, and high schools.
· Schools do not appear to have played a major role in COVID-19 transmission. In a review of COVID clusters, only 4% (8 of 210) involved school transmission.[5] In a case study from New South Wales Australia, after 18 cases were found in schools (12 in high schools and 6 in primary schools), only 0.3% of student contacts were infected (1 in 695 individuals in 10 high schools and 1 in 168 individuals in primary schools). No teachers or staff were infected.[6] Additional studies are included in Appendix A.
· In general, rates of COVID-19 infection are lower for children than for adults. Based on an analysis of data from six countries, children under 20 are half as susceptible to COVID-19 infection than adults.[7] Furthermore, although children under the age of 18 make up 22% of the U.S. population, they account for less than 2% of all cases of COVID-19.[8] In Massachusetts, children under the age of 19 were about four times less likely than the population at large to be diagnosed with COVID-19.[9] Children are more likely to be asymptomatic, however, which underscores the importance of health behaviors for everyone (masks/face coverings, distancing, handwashing, surface cleaning).[10] Additional studies are included in Appendix A.
· If exposed, children may be less likely to become infected with COVID-19. A meta-analysis of studies from several countries found that children were only 44% as likely as adults to become infected after exposure (note: pre-print study).[11] In China, in households with COVID-19 exposure, children under the age of 18 were infected at a rate of 4% compared with 17% for adults.[12] Additional studies are included in Appendix A.
· If infected, it appears children may be less likely to infect others with COVID-19. Most transmissions are from adults to children, rather than vice versa; this is different from some other respiratory viruses (note: pre-print study).[13] In a U.S. study of 15 households, 73% of transmissions were from adult to child (the remaining were child-to-child or child-to adult).[14] Additional studies are included in Appendix A.
Health and safety requirements and related guidance for in-person learning
The health and safety of students and staff are our top priority when making the decision to reopen schools for in-person learning in the fall. The following health and safety requirements have been developed in collaboration with infectious disease physicians, pediatricians and public health experts from the Massachusetts General Brigham Health System and the Massachusetts chapter of American Academy of Pediatrics. Our process has included a thorough review of guidelines from the Centers for Disease Control (CDC) and World Health Organization (WHO), as well as available medical literature on COVID-19 related to children and school settings. Finally, the MA COVID-19 Command Center Medical Advisory Board, made up of physicians and other health experts, has carefully reviewed the health and safety requirements for in-person learning outlined in this section.
At this time, these are the health and safety practices that will enable the safe reopening of schools for in-person learning this fall. These requirements will be modified as needed during the summer and into the fall. In addition to required practices, we have also included guidance on best practices where applicable.
As general background, COVID-19 spreads when people are in relatively close proximity, through respiratory droplets generated through coughing, sneezing, or talking to an infected person. Among the most effective preventive measures – when used consistently and in combination – are masks/face coverings, physical distancing, handwashing, and cleaning frequently touched surfaces.[15]
Masks/face coverings: As the primary route of transmission for COVID-19 is respiratory,[16] [17] [18] masks or face coverings are among the most critical components of risk reduction.[19] [20] [21] Masks/face coverings protect the general public against COVID-19 infection,[22] with a recent retrospective study estimating near 80% effectiveness in reducing COVID-19 transmission, especially when worn prior to symptom onset.[23] In the United States, states advising face masks/face coverings be worn in public saw a decline in their COVID-19 growth rates,24">[24] and community-wide mask/face covering usage contributed to control of COVID-19 in Hong Kong.[25] At this time, our initial requirements and related guidance are as follows:
● Students in grade 2 and above are required to wear a mask/face covering that covers their nose and mouth. Students in kindergarten and grade 1 should be encouraged to wear a mask/face covering.[26] Face shields may be an option for those students with medical, behavioral, or other challenges who are unable to wear masks/face coverings. Transparent masks may be the best option for both teachers and students in classes for deaf and hard of hearing students. They may also be useful for teachers and younger students who rely on visual / facial cues.
● Adults, including educators and staff, are required to wear masks/face coverings.
● Exceptions to mask/face covering requirements must be made for those for whom it is not possible due to medical conditions, disability impact, or other health or safety factors.
● Mask breaks should occur throughout the day.[27] Breaks should occur when students can be six feet apart and ideally outside or at least with the windows open. Further guidance on mask breaks including duration and frequency will be forthcoming, as well as more information about properly removing and putting on masks.
● Masks/face coverings should be provided by the student/family, but extra disposable face masks should be made available by the school for students who need them. Reusable masks/face coverings provided by families should be washed by families daily. Districts and schools with families experiencing financial hardship and unable to afford masks/face coverings should endeavor to provide masks for students through grant funds described earlier in this document.
● Masks/face coverings are required to be worn by everyone on the bus during school bus transportation.
● Transparent face coverings provide the opportunity for more visual cues and should be especially considered as an alternative for younger students, students who are deaf and hard of hearing, and their teachers.
Physical distancing: Physical distancing is another important practice that helps mitigate transmission of the virus. While the U.S. federal CDC has recommended maintaining a physical distance of six feet between individuals,[28] the World Health Organization’s guidance states approximately three feet.[29] There is no precise threshold for safety; indeed, studies suggest that physical distancing of three feet or more leads to reduced transmission, with additional distance providing additional protection.[30][31] For instance, in a study of household transmission in China, keeping at least three feet of distance was associated with one-fourth the number of transmissions.[32] It is important to note that six feet distancing is emphasized in public health advisories especially when no mask/face covering is worn.
We encourage districts and schools to aim for six feet of distance between individuals where feasible. At the same time, a minimum physical distance of three feet has been established when combined with the other measures outlined in this list of safety requirements. Because of the reduced susceptibility in children and lower apparent rates of transmission, establishing a minimum physical distance of three feet is informed by evidence and balances the lower risk of COVID-19 transmission and the overarching benefits of in-person school.
In preparing this document, we have reviewed the physical distance guidance for many other states and countries. In addition to the WHO, several other countries including Denmark, France, China, and Hong Kong recommend one meter (approximately three feet) distance in schools.[33] [34] [35] [36] The United Kingdom is also changing its guidance to one meter of distance beginning July 4, replacing previous guidance of two meters.[37]
Finally, this guidance is for fall reopening and is predicated on the Commonwealth continuing to progress through the phases of reopening with low COVID-19 public health metrics.[38] It will be critical to continue to take into account the community context of COVID-19 prevalence into the fall and winter. Where the community prevalence of COVID-19 is of concern, increased distancing will need to be considered.
Our initial requirements and related guidance are as follows:
● Distancing requirements: As reviewed and advised by the Massachusetts COVID-19 Command Center Medical Advisory Group, schools should aim for a physical distance of six feet when feasible, and three feet is the minimum distance allowed.[39] Schools should seek to maximize physical distance among individuals within their physical and operational constraints.
● Classroom and facility configuration: To the extent possible, aim for desks to be spaced six feet apart (but no fewer than three feet apart) and facing the same direction.40[40] Again, schools should seek to maximize physical distance between desks within their physical and operational constraints.
● Alternative spaces in the school (e.g., cafeteria, library, and auditorium) should be repurposed to increase the amount of available space to accommodate the maximum distance possible.
o In these larger spaces, establishing consistent cohorts/classes with separation between the cohorts/classes provides another option to maximize these spaces safely.
● Additional safety precautions are required for school nurses and/or any staff supporting students with disabilities in close proximity, when distance is not possible: These precautions must include eye protection (e.g., face shield or goggles) and a mask/face covering. Precautions may also include gloves and disposable gowns or washable outer layer of clothing depending on duration of contact and especially if the individual may come into close contact with bodily fluids.
Student groups: To minimize the number of students who would potentially be exposed in the event of a COVID-19 event, to the extent feasible, elementary schools should aim to keep students in the same group throughout the day and middle and high schools are encouraged to minimize mixing student groups to the extent feasible. Our initial requirements and related guidance are as follows:
· Cohorts: Schools should divide students into small groups that remain with each other throughout the day, with smaller cohort sizes preferred. Schools should look for ways to isolate cohorts of students and prevent inter-group contact to the extent feasible.
· Capacity: There are no required maximums on cohort or group sizes, so long as schools adhere to the physical distancing requirements above. (This guidance for the fall will replace previous summer guidance at the start of the school year, assuming positive health metrics hold.)
Screening upon entry: Checking for symptoms each morning by families and caregivers is critical and will serve as the primary screening mechanism for COVID-19 symptoms.[41] Schools should provide information to families in their primary language to support them in conducting this symptom check and families should not send their children to school if they exhibit COVID-19 symptoms. We will be providing a checklist of symptoms and other guides to districts and schools to help families and students.
· Screening procedures are not required at the point of entry to the school. However, school staff (as well as bus drivers) should observe students throughout the day and refer students who may be symptomatic to the school healthcare point of contact.
· As noted in previous guidance, temperature checks are not recommended as screening for all students due to the high likelihood of potential false positive and false negative results.[42]
Hand hygiene: Handwashing and hand sanitizing: Handwashing removes pathogens from the surface of the hands. While handwashing with soap and water is the best option, alcohol-based hand sanitizer (at least 60 percent ethanol or at least 70 percent isopropanol) may be utilized when handwashing is not available.[43] [44] As has always been the case, handwashing should be used whenever hands are visibly soiled and after using the bathroom.[45] Our initial requirements and related guidance are as follows:
· Students and staff are required to exercise hand hygiene (handwashing or sanitizing) upon arrival to school, before eating, before putting on and taking off masks, and before dismissal.
· Handwashing: When handwashing, individuals should use soap and water to wash all surfaces of their hands for at least 20 seconds, wait for visible lather, rinse thoroughly, and dry with an individual disposable towel.[46]
· Hand sanitizing: If handwashing is not feasible, hand sanitizer with at least 60 percent ethanol or at least 70 percent isopropanol content can be used.[47] Hand sanitizer should be applied to all surfaces of the hands and in sufficient quantity that it takes 20 seconds of rubbing hands together for the sanitizer to dry. Hand sanitizer should be placed at key locations (e.g., building entrances, cafeteria, classrooms).
COVID-19 related isolation space: In order to minimize transmission of COVID-19, schools must ensure they have an isolated space available for students displaying COVID-19 symptoms. Our initial requirements and related guidance are as follows:
· Schools are required to designate a COVID-19 related isolation space that is separate from the nurse’s office or other space where routine medical care is provided. A student who shows COVID-19 symptoms during the school day should be moved to the specific room pre-designated for medical-related isolation until they can be picked up by a family member.[48] More information about steps to safely discharge students will be provided in future guidance.
COVID-19 testing in schools: At this time, in-school testing is not recommended. Students’ families should discuss testing with their health care provider. As the accuracy of point-of-care testing develops, this guidance may change.
Vaccines: Districts and schools should work with parents to ensure that students are current on all standard vaccinations before they return to in-person school. In addition, health providers strongly recommend all students and staff get their regular flu vaccine.[49] Whereas for COVID-19 it appears children are less likely to be infected with and to transmit COVID-19, this is not the case for influenza, where children are frequent transmitters.50[50] [51] [52] [53] Therefore, ensuring all students, teachers, and staff receive the seasonal flu vaccine is an extremely high priority. The Department of Public Health will be issuing updated guidance regarding vaccines for schools and parents.
Health and safety/PPE supplies: Per the initial supply guidance issued by DESE, schools should have an inventory of standard healthcare supplies (e.g., masks and gloves). Use of additional supplies may be optional based on type of tasks performed (e.g., teachers do not need to wear gloves while teaching but may need to during necessary contact with students, such as when providing physical support to students with disabilities). All districts are eligible for federal CARES Act funds to support these purchases.
Additional health and safety protocols: Other protocols, such as facilities cleaning, are described later in this document.
District and school fall reopening plans
In this section, we describe the plans we are requiring all districts and schools to create to effectively prepare for fall reopening. This section also offers recommendations on reopening models to support districts and schools in preparing these plans.
Components of district/school fall reopening plans
Each district and school will need to plan for three possibilities on the continuum of reopening: 1) in-person learning with new safety requirements; 2) a hybrid of in-person and remote learning; and 3) remote learning. In addition, all districts/schools will also need a focused plan for serving special student populations across each of these models.


1. In-person learning with new safety requirements: For the fall, the box in light blue represents our goal to get as many students as possible back into schools for in-person learning—safely. In this model, all students return in person to school settings that are appropriately modified to accommodate the health and safety requirements outlined above. Examples of modifications could include altered classroom configurations, setting up additional learning spaces, and schedule changes.
2. Hybrid learning: In addition, all districts/schools must create a plan for a hybrid model in the event they are unable to bring all students back to school under the health and safety requirements despite their best efforts, or in case of COVID-19 related circumstances. A hybrid model means that students would alternate between in-person and remote learning. For instance, students could switch between in-person and remote learning on alternating weeks or days of the week.
3. Remote learning: All districts and schools are required to have a plan for operating a remote learning program. This model must be available for individual students who cannot yet return in-person, and for all students in the event of future classroom or school closures due to COVID-19. Additional guidance on statewide support and resources for remote learning will be provided in the coming weeks.
Plan for special populations: Finally, across each of these models, all districts and schools need a plan for how special populations, including students with disabilities and English learners, will receive necessary services and accommodations.
Plan development and submission
Districts and schools will be required to submit their comprehensive fall reopening plans (all three models) to DESE in August. In addition, districts and schools will need to post their plans on their websites and complete an attestation to affirm that their fall reopening plans meet the health and safety guidelines established in this and updated guidance documents. We will issue further guidance, including whether any portions of the plans will require approval by DESE (for instance, plans for students with disabilities or others).
In creating their plans, districts and schools should first prioritize developing an in-person learning model with new safety requirements. DESE staff will establish multiple communications channels with superintendents and other school stakeholders to monitor how planning for an in-person return to school is progressing. We recognize the importance of equity in this process and will be available to support districts and schools in troubleshooting challenges that may arise.
Recommendations from DESE on reopening models
The model recommendations below assume key contextual factors that are not within our collective control. This includes an assumption of “level service plus” district and school budgets based on current projections, which include additional costs that may come with modifying class sizes, staffing, transportation, facilities, etc. We also recognize that “level service plus” must include additional resources targeted to historically under-resourced communities. The trajectory of the virus and availability of testing and treatments are other critical contextual factors. We will continue to monitor these and other factors and issue updated guidance as needed.
In-person learning with new safety requirements:
Learning time: Districts and schools should plan for an in-person return to school five days per week if feasible.
Utilizing alternative school spaces: Districts and schools should consider using their libraries, cafeterias, auditoriums, and other appropriate available spaces to set up additional classrooms to accommodate more students, reduce class size, and/or enable additional distancing while adhering to the health and safety guidelines. Teachers may also hold classes outdoors when feasible.
Utilizing external facility spaces: Schools should consider engaging community partners to find spaces outside the school[54] (e.g., libraries, community centers) to set up additional classrooms[55] to accommodate more students, reduce class size, and/or enable additional distancing while adhering to the health and safety guidelines.
Staffing alternatives to consider for reducing class sizes: Specialist teachers and other educators such as instructional coaches, reading specialists, and others who have appropriate certifications may be enlisted to serve as additional core teachers to reduce class sizes in schools.
Reducing the mixing of student groups: When in classrooms, all students should have assigned seating. At the elementary school level, students should be restricted to their grade level class to the greatest extent possible. At the middle school level, students should remain with their cohort throughout the day to the extent feasible.
High schools could also consider ways to cohort or cluster students, though we recognize this is more challenging at the high school level:
· Placing students in cohorts. When grouping students into cohorts, a school should consider ways to keep families/siblings together (e.g., grouping students alphabetically, while recognizing that some siblings may have different last names).
· Limiting travel within a school. High schools may try to group students into clusters in the school (a “school within a school”) to try to reduce interactions with other groups when students move to their next class.
Hybrid learning models:
When planning for a hybrid learning model, we recommend that districts and schools use an A/B cohort model that isolates two distinct cohorts of students who attend school in-person on either different weeks, different days of the week, or half days each day. For instance, Cohort A would attend school in-person from Monday – Friday of Week 1, while Cohort B learns at home remotely. In Week 2, Cohort B would attend in-person school and Cohort A would engage in remote learning at home.
Additional recommendations for hybrid models include:
High-needs students should be prioritized for full-time in-person learning when feasible. That is, even if most students are not in school each day, schools should consider setting up small programs that would run daily for one or more cohorts of high-needs students, including students with disabilities and English learners who are most in need of in-person services.
Students who do not have internet and/or computer access at home should come into the school and/or to a local partner or community organization, with appropriate supervision, to complete their remote learning school days.
Initial fall reopening planning steps
This section provides a checklist of key actions districts and schools should take in the coming weeks to plan for all three fall reopening models. This list focuses on establishing processes and communication structures; future guidance will have more details about concrete operational planning.[56] Please see Appendix B and C of this document for initial operational guidance for the fall in a few areas (facilities, operations, and special education).
Point person and teams:
ü Name a COVID-19 response leader. If you have not done so already, name a COVID-19 Response Leader for each school and for the district. The COVID-19 response leaders should coordinate with key district and school personnel on planning efforts over the summer and be a key part of the implementation as schools open.
ü Establish planning and implementation teams at the district and school levels to work intensively over the summer on all issues related to school reopening in the fall. Planning and implementation teams should include COVID-19 response leaders, district leaders, school administrators, general and special education teaching staff, school nurses, custodial staff, as well as parents and other local officials and organizations as appropriate. These teams should cover the following essential domains:
o Teaching and learning, including plans for in-person learning, hybrid learning, and remote learning, including technology needs and training.
o Student supports, including addressing mental health and trauma.
o Special education, English learners, and other special student populations.
o Personnel and staffing, including managing staff assignments, supporting staff with high risk medical conditions, addressing the need for possible additional staff to assist with instruction, possible additional needs for tutors, and ways to provide additional support including recruitment of volunteers as needed.
o Facilities and operations, including cleaning and sanitation, classroom and building set-up and flow, and food services.
o Transportation, including bus transportation capacity and safety protocols, management of increased traffic flow from families who decide to drop off/pick up their children, promotion of alternatives such as walking and biking.
o Additional topics should be addressed as appropriate to the school and the district.
Communication plans and structures:
ü Develop and begin implementing this summer a plan for communicating more intensively with students, families, staff, and the community. This plan should include both two-way proactive communication (e.g., providing information and receiving feedback) and emergency communication. Consider creating and practicing communication systems with parents, students, all staff, facility and/or grounds management, and emergency medical services. Ensure translation of any information published by the school into the primary language spoken by the parent/guardian and make interpretation services available for two-way communication.
ü Establish connections and a process to work with local boards of health so that all parties are up to date on various statewide and local guidance and plans (e.g., health and safety updates, COVID-19 testing availability, availability of flu vaccines, etc.).
Family survey:
ü Develop a family survey to support school reopening planning and scheduling. Districts should consider surveying families multiple times throughout the summer and potentially into the school year. Districts and schools can use the survey to help determine:
· Children who will return to school in the fall in-person
· Children who will continue remote learning and for what reasons
· Children who need internet/technology access, and/or other technical support or one-on-one guidance
· Children who will need bus transportation
· Families who are planning to use alternate transportation (e.g., drop off and pick up their children, have their children walk or bike)
· Families who will need food assistance and other essential services
Planning for training:
ü Build in time in the fall calendar for training sessions for staff, students, and families. Training should include health and safety topics (such as the use of safety supplies/PPE, visual screening for symptoms, and health and hygiene practices) and educational topics (such as strengthening remote learning). More guidance will be forthcoming.
ü Special education: Ensure additional training time for educators who will provide direct physical support to students with disabilities on the use of the additional protective supplies they will need, including disposable gowns, face shields, etc.
Timing and topics for additional guidance
As districts and schools begin planning in earnest for fall reopening, DESE is committed to supporting you. In the coming weeks, we will issue more guidance on a variety of topics for the fall. We will also continue to update our guidance based on evolving medical information and contextual factors.
Below is list of additional topics on which DESE intends to issue guidance:
·
Remote learning resources. We are actively exploring how best to support districts and schools with improving remote learning.
·
·
Key policies, including academic calendar considerations.
Supplemental guidance for vocational high schools and programs will also be forthcoming.
Appendix A: Details on medical literature review and emerging implications
This section summarizes some of the emerging themes and implications from the medical literature on childhood susceptibility to and transmission of COVID-19 to date. This is a point-in-time summary as of mid-June 2020.
The evidence suggests that children, particularly younger children, are less likely than adults to be infected with COVID-19. Furthermore, if infected, children may be less likely to transmit COVID-19 to others.
Based on these themes, the health and safety recommendations throughout this guidance, as well as considering the key features of school programming at different grade spans, we believe the evidence supports a safe in-person return to school with implementation varying for elementary, middle school, and high school.
Because COVID-19 is a novel disease, this literature is growing rapidly with new information emerging almost every day. Our guidance will continue to evolve as the science develops.
Schools do not appear to have played a major role in COVID-19 transmission.
· In a review of COVID-19 clusters, only 4% (8 of 210) involved school transmission.[57]
· In a case study from Ireland, after six school cases involving three students ages 10-15 and three adults, there were no confirmed transmissions despite there being over 1,000 school contacts of these individuals (students and staff).[58]
· In a case study from New South Wales Australia, after 18 cases were found in schools (12 in high schools and 6 in primary schools), only 0.3% of student contacts were infected (1 in 695 individuals in 10 high schools and 1 in 168 individuals in primary schools). No teachers or staff were infected.[59]
· One infected student (9 years old) in the French Alps attended three schools while symptomatic; none of 112 contacts became infected.60[60]
In general, rates of COVID-19 infection are lower for children than for adults.
· Based on data from six countries, children under 20 are half as susceptible to COVID-19 infection than adults.[61] However, this study also found infection in children to be more likely to be asymptomatic, which underscores the importance of health behaviors for everyone (masks/face coverings, distancing, handwashing, surface cleaning).
· Although children under the age of 18 make up 22% of the U.S. population, they account for less than 2% of all cases of COVID-19.[62]
· In a South Korea study, children under 20 only accounted for 6.2% of all positive cases.[63]
· After an outbreak in Italy, no children under 10 were infected and children 11-20 were infected at half the overall rate.[64] (Note: pre-print study; has not yet been peer-reviewed)
· In a Chicago study, only 1% of COVID-19 cases in Chicago were in children 0-17.[65]
· In Massachusetts, children under the age of 19 were about four times less likely than the population at large to be diagnosed with COVID-19.[66]
If exposed, children may be less likely to become infected with COVID-19.
· In China, in households with COVID-19 exposure, children under the age of 18 were infected at a rate of 4% compared with 17% for adults.[67]
· In another study from China, exposed children less than 19 years of age became infected at a rate of 5.3%, vs. 13.7% for 20-59 and 17.7% for 60+.[68] (Note: pre-print study; has not yet been peer-reviewed)
· In one study from Japan, 7.2% of exposed male children ages 0-19 and 3.8% of exposed female children tested positive for COVID-19, compared to 22.2% of exposed males ages 20-59 and 21.9% of exposed females ages 20-59.[69] (Note: pre-print study; has not yet been peer-reviewed)
· In NYC, in households with at least one COVID-19 case, prevalence of infection for children 5-≤18 was 31.9% vs. overall prevalence 52.5%.70[70]
· A meta-analysis of studies from several countries found that children were only 44% as likely as adults to become infected after exposure.[71] (Note: pre-print study; has not yet been peer-reviewed)
· A study in Israel found that children 5-17 were 61% less likely to have positive COVID-19 tests compared with adults in the same household.[72]
If infected, children may be less likely to infect others with COVID-19.
· Analysis of clusters of patients with COVID-19 indicates that most transmissions are from adults to children, rather than vice versa. This is different from some other respiratory viruses.[73] (Note: pre-print study; has not yet been peer-reviewed)
· In a study from China, only 5% of household clusters were found to have a child <20 as the index patient.[74] (Note: pre-print study; has not yet been peer-reviewed)
· In Switzerland, a study of household clusters found that only 8% had a child as the index case. In nearly 80% of the cases, the child got COVID-19 from an adult family member.[75]
· In a Chicago study, for 15 households where data was available, 73% of transmissions were from adult to child (the remaining 27% was due to two child-to-child and two child-to adult transmissions).[76]
Risk of infection at varying physical distances
Key finding: in intermediate- and low-risk settings, the risk of infection is similar at one meter (approximately three feet) and two meters (approximately six feet) distances. Experts suggest schools would be considered low to intermediate risk, especially with additional protections (e.g., masks), and that the risk of infection in these settings at both one meter and two meters is low.
Note: the risk of infection at various physical distances was modeled based on a meta-analysis of data from a group of coronaviruses (COVID-19, MERS, SARS). These are estimates of the risk by type of setting, not the risk to different types of individuals.
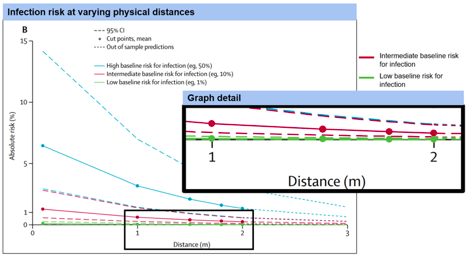

Source: Chu, D.K., Akl, E.A., Duda S., Solo K., Yaacoub S., Schunemann H.J. et al. (2020) Physical distancing, face masks, and eye protection to prevent person-to-person transmission of SARS-CoV-2 and COVID-19: a systematic review and meta-analysis. The Lancet.
Appendix B: Initial list of facilities and operations guidance
The considerations below are not exhaustive but can be used to support districts and schools with early operational planning in these areas.
Cleaning and supplies: Prepare for frequent cleaning and sanitization of facilities and surfaces, especially high-touch surfaces (e.g., doorknobs, hand rails).[77] [78] Please refer to the federal guidance related to cleaning of facilities for more information regarding appropriate cleaning supplies, protocols, and frequency (e.g., wear appropriate protection such as gloves, wash hands often, follow instructions on all cleaning products, handle waste properly).[79] 80[80] Provide hand sanitizing at key locations in the building (e.g., entryways, bathrooms, classrooms). Install signage and equipment to enable effective health and safety procedures, as defined in the Commonwealth’s guidance on required safety supplies for reopening schools.
Facility management: Prepare an “medical isolation room” for students/staff who exhibit COVID-19 symptoms during the school day.[81] Consider removing large furniture (e.g., refrigerator, couches) from classrooms to maximize space available for student desks, and ensure desks are spaced according to the physical distancing guidance and facing in same direction, to reduce the transmission of droplets. Where physical distancing is difficult to implement (e.g., office space, reception desks), consider installing barriers or changing the configuration to support student/staff health and safety.[82] Repurpose communal spaces (e.g., cafeteria, library) to provide additional classroom spaces. If feasible, redesign hallways to be one-way to avoid crowding or restrict usage where distancing is not possible. Establish procedures for student entry and dismissal from the building.
Capacity: Evaluate classroom capacity on a case-by-case basis, based on the maximum capacity consistent with health and safety guidelines (e.g., distancing). Remember to include adequate space for the teachers. For the overall facility, plan for traffic, drop off, and pick up (e.g., staggered pickup/dismissal as needed).
Ventilation: Consider ways to increase facility ventilation (e.g., open windows through fall, perform an HVAC inspection)[83]. Ensure that proper maintenance protocols are followed in terms of changing filters, etc.
Food: Prepare to hold breakfast and/or lunch in classrooms, instead of the cafeteria or common areas.[84] As it is assumed that masks/face coverings will not be worn during meals, in order to achieve six feet of physical distance between individuals, consider ways to conduct breakfast and lunch (e.g., stagger time, build in other breaks, etc.). If serving food in the cafeteria, develop staggered schedules that minimize mixing of cohorts and enforce physical distancing protocols. Adjust food preparation and service procedures to minimize shared items (i.e. serving utensils), maintain physical distance, and support compliance with health and safety. For students continuing with remote learning, provide school meals as needed for days they are not in the school building.
Appendix C: Initial Fall Special Education Guidance
Due to the health and safety requirements that will be in place when school resumes, special education services may be provided differently during the 2020-21 school year as compared to previous years. As stated in the U.S. Department of Education’s March 21 Supplemental Fact sheet, “School districts must provide a free and appropriate public education (FAPE) consistent with the need to protect the health and safety of students with disabilities and those individuals providing education, specialized instruction, and related services to these students.” While further guidance is forthcoming, the topics listed below are meant to support school and district special education leaders in their initial plans for the new school year.
Promoting Inclusive Services and the Least Restrictive Environment
When determining classroom setups to accommodate physical distancing requirements, schools and districts should factor in the additional special educators and related service providers who will need to enter the classroom to provide services for students with disabilities in the least restrictive environment.
Staffing, Specialized Safety Supplies/PPE and Training
Schools and districts should follow the directions for staffing, specialized safety supplies/PPE and training described in DESE’s Guidance on Summer 2020 Special Education Services as they prepare for this fall.
Considerations for Specific Populations of Students
Special considerations must be given for students with high risk medical conditions, students who are deaf or hard of hearing, and preschool-age students. Additional directions can be found in DESE’s Guidance on Summer 2020 Special Education Services.
Considerations for Preschool-Age Students
Preschool-age students with disabilities are particularly in need of in-person services so that they can develop the socialization, motor, and communication skills that are vitally important at this age. Schools and districts should prioritize in-person instruction for this age group but should also be prepared to adjust to remote services if necessary.
Delivery of IEP Services
Students must receive all services pursuant to their IEPs through in-person or remote instruction, with an emphasis on providing in-person instruction to this particularly vulnerable population of students whenever possible. In particular, DESE recommends that schools and districts make additional provisions to provide as much in-person instruction as possible for students with moderate to severe disabilities (e.g., maintaining full-time in-person instruction for students in substantially separate classrooms even if the rest of the school is in a hybrid model of instruction). When providing remote services, schools and districts should continue to follow the directions provided in DESE’s Coronavirus/COVID-19 Frequently Asked Questions for Schools and Districts Regarding Special Education (Updated May 15, 2020).
Monitoring Student Progress
Schools and districts must continue to issue Progress Reports at least as often as report cards or progress reports are provided for students without disabilities. Educators and service providers must collect data, whether in-person or remotely, and use these data to monitor each student’s progress and develop Progress Reports.
Transition Services
Although in-person participation in community-based programs and inclusive concurrent enrollment programs at institutions of higher education may be limited at this time, schools and districts should make efforts to develop plans collaboratively with community-based providers, colleges, parents/guardians, and students so that students can access as much programming as possible.
Initial Evaluations, Reevaluations, and IEP Team Meetings
Schools and districts should continue to follow the directions on meeting special education timelines as described in DESE’s Implementation of Special Education Timelines During the COVID-19 State of Emergency.
Communication with Families
Educators and service providers must communicate with parents and guardians to discuss the provision of IEP services during this challenging time. Ongoing communication will help educators, related service providers, and parents/guardians develop a comprehensive plan for students to receive high quality individualized instruction and related services.
ref[1] Leclerc, Q. J., Fuller, N. M., Knight, L. E., Funk, S., Knight, G. M., & CMMID COVID-19 Working Group. (2020). What settings have been linked to SARS-CoV-2 transmission clusters?. Wellcome Open Research, 5(83), 83. Available at https://wellcomeopenresearch.org/articles/5-83/v2
ref[2] Heavey, L., Casey, G., Kelly, C., Kelly, D., & McDarby, G. (2020). No evidence of secondary transmission of COVID-19 from children attending school in Ireland, 2020. Eurosurveillance, 25(21), 2000903. Available at https://www.eurosurveillance.org/content/10.2807/1560-7917.ES.2020.25.21.2000903
ref[3] National Centre for Immunisation Research and Surveillance (NCIRS) (2020). COVID-19 in schools – the experience in NSW. Available at http://ncirs.org.au/sites/default/files/2020-04/NCIRS%20NSW%20Schools%20COVID_Summary_FINAL%20public_26%20April%202020.pdf
ref[4] Danis, K., Epaulard, O., Bénet, T., Gaymard, A., Campoy, S., Bothelo-Nevers, E., ... & Boudalaa, Z. (2020). Cluster of coronavirus disease 2019 (Covid-19) in the French Alps, 2020. Clinical Infectious Diseases. Available at https://academic.oup.com/cid/advance-article/doi/10.1093/cid/ciaa424/5819060
ref5" name="_edn[5] Leclerc, Q. J., Fuller, N. M., Knight, L. E., Funk, S., Knight, G. M., & CMMID COVID-19 Working Group. (2020). What settings have been linked to SARS-CoV-2 transmission clusters?. Wellcome Open Research, 5(83), 83. Available at https://wellcomeopenresearch.org/articles/5-83/v2
ref6" name="_edn[6] National Centre for Immunisation Research and Surveillance (NCIRS) (2020). COVID-19 in schools – the experience in NSW. Available at http://ncirs.org.au/sites/default/files/2020-04/NCIRS%20NSW%20Schools%20COVID_Summary_FINAL%20public_26%20April%202020.pdf
ref7" name="_edn[7] Davies, N.G., Klepac, P., Liu, Y. et al. Age-dependent effects in the transmission and control of COVID-19 epidemics. Nat Med (2020). https://doi.org/10.1038/s41591...
ref8" name="_edn[8] Coronavirus Disease 2019 in Children — United States, February 12–April 2, 2020. MMWR Morb Mortal Wkly Rep 2020;69:422–426. DOI: http://dx.doi.org/10.15585/mmwr.mm6914e4
ref9" name="_edn[9] https://www.mass.gov/info-details/covid-19-response-reporting
ref10" name="_edn[10] Davies, N.G., Klepac, P., Liu, Y. et al. Age-dependent effects in the transmission and control of COVID-19 epidemics. Nat Med (2020). https://doi.org/10.1038/s41591...
ref11" name="_edn[11] Viner, R. M., Mytton, O. T., Bonell, C., Melendez-Torres, G. J., Ward, J. L., Hudson, L., ... & Panovska-Griffiths, J. (2020). Susceptibility to and transmission of COVID-19 amongst children and adolescents compared with adults: a systematic review and meta-analysis. medRxiv. Available at https://www.medrxiv.org/content/10.1101/2020.05.20.20108126v1
ref12" name="_edn[12] Wei Li, Bo Zhang, Jianhua Lu, Shihua Liu, Zhiqiang Chang, Cao Peng, Xinghua Liu, Peng Zhang, Yan Ling, Kaixiong Tao, Jianying Chen, Characteristics of Household Transmission of COVID-19, Clinical Infectious Diseases, , ciaa450, https://doi.org/10.1093/cid/ciaa450
ref13" name="_edn[13] Zhu, Y., Bloxham, C. J., Hulme, K. D., Sinclair, J. E., Tong, Z. W. M., Steele, L. E., ... & Gilks, C. (2020). Children are unlikely to have been the primary source of household SARS-CoV-2 infections. Available at https://www.medrxiv.org/content/10.1101/2020.03.26.20044826v1
ref14" name="_edn[14] Mannheim, J., Gretsch, S., Layden, J. E., & Fricchione, M. J. (2020). Characteristics of Hospitalized Pediatric COVID-19 Cases—Chicago, Illinois, March–April 2020. Journal of the Pediatric Infectious Diseases Society. Available at https://academic.oup.com/jpids/advance-article/doi/10.1093/jpids/piaa070/5849922
ref15" name="_edn[15] CDC, How COVID-19 spreads. (2020, June 16). Available at https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/how-covid-spreads.html
ref16" name="_edn[16] Zhang, Renyi, et al. "Identifying airborne transmission as the dominant route for the spread of COVID-19." Proceedings of the National Academy of Sciences (2020).
ref17" name="_edn[17] CDC., et al. "Coronavirus Disease 2019 in Children—United States, February 12–April 2, 2020." Morbidity and Mortality Weekly Report 69.14 (2020): 422.
ref18" name="_edn[18] World Health Organization. Modes of transmission of virus causing COVID-19: implications for IPC precaution recommendations: scientific brief, 27 March 2020. No. WHO/2019-nCoV/Sci_Brief/Transmission_modes/2020.1. World Health Organization, 2020. Available at: https://www.who.int/news-room/commentaries/detail/modes-of-transmission-of-virus-causing-covid-19-implications-for-ipc-precaution-recommendations
ref19" name="_edn[19] Wang, Y., Tian, H., Zhang, L., Zhang, M., Guo, D., Wu, W., ... & Liu, B. (2020). Reduction of secondary transmission of SARS-CoV-2 in households by face mask use, disinfection and social distancing: a cohort study in Beijing, China. BMJ Global Health, 5(5), e002794. Available at https://gh.bmj.com/content/bmjgh/5/5/e002794.full.pdf
ref20" name="_edn[20] Lyu, W. and Wehby, G. L. (2020). Community Use Of Face Masks And COVID-19: Evidence From A Natural Experiment Of State Mandates In The US. Health Affairs. Available at https://doi.org/10.1377/hlthaf...
ref21" name="_edn[21] Cheng, V. C., Wong, S. C., Chuang, V. W., So, S. Y., Chen, J. H., Sridhar, S., ... & Yuen, K. Y. (2020). The role of community-wide wearing of face mask for control of coronavirus disease 2019 (COVID-19) epidemic due to SARS-CoV-2. Journal of Infection. Available at https://www.journalofinfection.com/article/S0163-4453(20)30235-8/pdf
ref22" name="_edn[22] Chu, D.K., Akl, E.A., Duda S., Solo K., Yaacoub S., Schunemann H.J. (2020) Physical distancing, face masks, and eye protection to prevent person-to-person transmission of SARS-CoV-2 and COVID-19: a systematic review and meta-analysis. The Lancet
ref23" name="_edn[23] Wang, Y., Tian, H., Zhang, L., Zhang, M., Guo, D., Wu, W., ... & Liu, B. (2020). Reduction of secondary transmission of SARS-CoV-2 in households by face mask use, disinfection and social distancing: a cohort study in Beijing, China. BMJ Global Health, 5(5), e002794. Available at https://gh.bmj.com/content/bmjgh/5/5/e002794.full.pdf
ref24" name="_edn[24] Lyu, W. and Wehby, G. L. (2020). Community Use Of Face Masks And COVID-19: Evidence From A Natural Experiment Of State Mandates In The US. Health Affairs. Available at https://doi.org/10.1377/hlthaf...
ref25" name="_edn[25] Cheng, V. C., Wong, S. C., Chuang, V. W., So, S. Y., Chen, J. H., Sridhar, S., ... & Yuen, K. Y. (2020). The role of community-wide wearing of face mask for control of coronavirus disease 2019 (COVID-19) epidemic due to SARS-CoV-2. Journal of Infection. Available at https://www.journalofinfection.com/article/S0163-4453(20)30235-8/pdf
ref26" name="_edn[26] http://www.sickkids.ca/PDFs/About-SickKids/81407-COVID19-Recommendations-for-School-Reopening-SickKids.pdf (if masks are worn incorrectly, they may increase infection risk). See also: https://www.publichealthontario.ca/-/media/documents/ncov/covid-wwksf/what-we-know-public-masks-apr-7-2020.pdf?la=en
ref27" name="_edn[27] Chu, D.K., Akl, E.A., Duda S., Solo K., Yaacoub S., Schunemann H.J. (2020) Physical distancing, face masks, and eye protection to prevent person-to-person transmission of SARS-CoV-2 and COVID-19: a systematic review and meta-analysis. The Lancet (the challenges of constant mask wearing include “frequent discomfort”)
ref28" name="_edn[28] CDC, Social Distancing, Quarantine, and Isolation. (2020, May 6). Retrieved from https://www.cdc.gov/coronavirus/2019-ncov/prevent-getting-sick/social-distancing.html
ref29" name="_edn[29] WHO, Considerations for school-related public health measures in the context of COVID-19. (2020, May 10). Available at https://www.who.int/publications/i/item/considerations-for-school-related-public-health-measures-in-the-context-of-covid-19
ref30" name="_edn[30] Chu, D.K., Akl, E.A., Duda S., Solo K., Yaacoub S., Schunemann H.J. (2020) Physical distancing, face masks, and eye protection to prevent person-to-person transmission of SARS-CoV-2 and COVID-19: a systematic review and meta-analysis. The Lancet
ref31" name="_edn[31] Zhang, J., Litvinova, M., Liang, Y., Wang, Y., Wang, W., Zhao, S., ... & Ajelli, M. (2020). Changes in contact patterns shape the dynamics of the COVID-19 outbreak in China. Science. Available at https://science.sciencemag.org/content/early/2020/05/04/science.abb8001
ref32" name="_edn[32] Wang, Y., Tian, H., Zhang, L., Zhang, M., Guo, D., Wu, W., ... & Liu, B. (2020). Reduction of secondary transmission of SARS-CoV-2 in households by face mask use, disinfection and social distancing: a cohort study in Beijing, China. BMJ Global Health, 5(5), e002794. Available at https://gh.bmj.com/content/bmjgh/5/5/e002794.full.pdf
ref33" name="_edn[33] Denmark National Board of Health, COVID-19: Prevention of infection spread. (2020, May 10). Available at https://www.sst.dk/da/Udgivelser/2020/COVID-19-Forebyggelse-af-smittespredning
ref34" name="_edn[34] France Ministère de l'Éducation Nationale et de la Jeunesse, Accueil de tous les élèves des écoles et collèges. (2020, June 22). Available at https://www.education.gouv.fr/22-juin-accueil-de-tous-les-eleves-des-ecoles-et-colleges-303546
ref35" name="_edn[35] Hong Kong Education Bureau. Guidelines to Schools on Class Resumption. (2020, June 16). Available at https://www.edb.gov.hk/attachment/en/sch-admin/admin/about-sch/diseases-prevention/Guidelines%20to%20Schools%20on%20Class%20Resumption%20(E).pdf
ref36" name="_edn[36] Washington Post. Two meters? One meter plus? Social distancing rules prompt fierce debate in U.K. (2020, June 22). Available at https://www.washingtonpost.com/world/europe/covid-social-distancing-one-meter-plus/2020/06/22/7614418a-afe0-11ea-98b5-279a6479a1e4_story.html
ref37" name="_edn[37] Telegraph. 'One metre plus', the new rule that will reopen UK. (2020, June 20). Available at https://www.telegraph.co.uk/po...
ref38" name="_edn[38] Reopening Massachusetts plan, https://www.mass.gov/info-details/reopening-massachusetts
ref39" name="_edn[39] WHO, Considerations for school-related public health measures in the context of
COVID-19. (2020, May 10). Available at https://www.who.int/publications/i/item/considerations-for-school-related-public-health-measures-in-the-context-of-covid-19
ref40" name="_edn[40] CDC, Considerations for Schools. (2020, May 19). Available at https://www.cdc.gov/coronavirus/2019-ncov/community/schools-childcare/schools.html
ref41" name="_edn[41] CDC, Considerations for Schools. (2020, May 19). Available at https://www.cdc.gov/coronavirus/2019-ncov/community/schools-childcare/schools.html
ref42" name="_edn[42] Asadian, Simin, et al. "Accuracy and precision of four common peripheral temperature measurement methods in intensive care patients." Medical Devices (Auckland, NZ) 9 (2016): 301.
ref43" name="_edn[43] CDC, Hand Hygiene Recommendations. (2020, May 17). Available at https://www.cdc.gov/coronavirus/2019-ncov/hcp/hand-hygiene.html
ref44" name="_edn[44] Kratzel, A., Todt, D., V'kovski, P., Steiner, S., Gultom, M., Thao, T. T. N., ... & Dijkman, R. (2020). Inactivation of severe acute respiratory syndrome coronavirus 2 by WHO-recommended hand rub formulations and alcohols. Emerg Infect Dis, 26. Available at https://wwwnc.cdc.gov/eid/article/26/7/20-0915_article
ref45" name="_edn[45] CDC, Hand Sanitizer Use Out and About. (2020, April 13). Available at https://www.cdc.gov/handwashing/hand-sanitizer-use.html
ref46" name="_edn[46] CDC, Hand Hygiene Recommendations, (2020, May 17). Available at https://www.cdc.gov/coronavirus/2019-ncov/hcp/hand-hygiene.html
ref47" name="_edn[47] CDC, Hand Hygiene Recommendations, (2020, May 17). Available at https://www.cdc.gov/coronavirus/2019-ncov/hcp/hand-hygiene.html
ref48" name="_edn[48] CDC, Considerations for Schools. (2020, May 19). Available at https://www.cdc.gov/coronavirus/2019-ncov/community/schools-childcare/schools.html
ref49" name="_edn[49] Gostin L. O., Salmon D. A. The Dual Epidemics of COVID-19 and Influenza: Vaccine Acceptance, Coverage, and Mandates. JAMA. Published online June 11, 2020. doi:10.1001/jama.2020.10802
ref50" name="_edn[50] Worby, C. J., Chaves, S. S., Wallinga, J., Lipsitch, M., Finelli, L., & Goldstein, E. (2015). On the relative role of different age groups in influenza epidemics. Epidemics, 13, 10-16. Available at https://www.sciencedirect.com/science/article/pii/S1755436515000511
ref51" name="_edn[51] White, L. F., Archer, B., & Pagano, M. (2014). Determining the dynamics of influenza transmission by age. Emerging themes in epidemiology, 11(1), 4. Available at https://link.springer.com/article/10.1186/1742-7622-11-4
ref52" name="_edn[52] Caini, S., Spreeuwenberg, P., Kusznierz, G. F., Rudi, J. M., Owen, R., Pennington, K., ... & Njouom, R. (2018). Distribution of influenza virus types by age using case-based global surveillance data from twenty-nine countries, 1999-2014. BMC infectious diseases, 18(1), 1-10. Available at https://bmcinfectdis.biomedcentral.com/articles/10.1186/s12879-018-3181-y
ref53" name="_edn[53] Tokars, J. I., Olsen, S. J., & Reed, C. (2018). Seasonal incidence of symptomatic influenza in the United States. Clinical Infectious Diseases, 66(10), 1511-1518. Available at https://academic.oup.com/cid/a...
ref54" name="_edn[54] Oregon Department of Education, Ready Schools, Safe Learners, Guidance for School Year 2020-21 (June 10, 2020). Available at https://www.oregon.gov/ode/students-and-family/healthsafety/documents/ready%20schools%20safe%20learners%202020-21%20guidance.pdf
ref55" name="_edn[55] Spaces4learning, Thinking Outside The Box: Adaptive Reuse For Education (November, 2019). Available at https://spaces4learning.com/Articles/2019/11/01/Adaptive-Reuse-For-Education.aspx?Page=2
ref56" name="_edn[56] For example, see: Massachusetts Department of Early Education and Care, Massachusetts Child and Youth Serving Programs Reopen Approach: Minimum Requirements for Health and Safety (pg. 6-8) https://eeclead.force.com/resource/1592325278000/Min_Req
ref57" name="_edn[57] Leclerc, Q. J., Fuller, N. M., Knight, L. E., Funk, S., Knight, G. M., & CMMID COVID-19 Working Group. (2020). What settings have been linked to SARS-CoV-2 transmission clusters?. Wellcome Open Research, 5(83), 83. Available at https://wellcomeopenresearch.org/articles/5-83/v2
ref58" name="_edn[58] Heavey, L., Casey, G., Kelly, C., Kelly, D., & McDarby, G. (2020). No evidence of secondary transmission of COVID-19 from children attending school in Ireland, 2020. Eurosurveillance, 25(21), 2000903. Available at https://www.eurosurveillance.org/content/10.2807/1560-7917.ES.2020.25.21.2000903
ref59" name="_edn[59] National Centre for Immunisation Research and Surveillance (NCIRS) (2020). COVID-19 in schools – the experience in NSW. Available at http://ncirs.org.au/sites/default/files/2020-04/NCIRS%20NSW%20Schools%20COVID_Summary_FINAL%20public_26%20April%202020.pdf
ref60" name="_edn[60] Danis, K., Epaulard, O., Bénet, T., Gaymard, A., Campoy, S., Bothelo-Nevers, E., ... & Boudalaa, Z. (2020). Cluster of coronavirus disease 2019 (Covid-19) in the French Alps, 2020. Clinical Infectious Diseases. Available at https://academic.oup.com/cid/advance-article/doi/10.1093/cid/ciaa424/5819060
ref61" name="_edn[61] Davies, N.G., Klepac, P., Liu, Y. et al. Age-dependent effects in the transmission and control of COVID-19 epidemics. Nat Med (2020). https://doi.org/10.1038/s41591...
ref62" name="_edn[62] Coronavirus Disease 2019 in Children — United States, February 12–April 2, 2020. MMWR Morb Mortal Wkly Rep 2020;69:422–426. DOI: http://dx.doi.org/10.15585/mmwr.mm6914e4
[63] Coronavirus Disease-19: The First 7,755 Cases in the Republic of Korea. Osong Public Health Res Perspect. 2020;11(2):85-90. Published online April 30, 2020. DOI: https://doi.org/10.24171/j.phrp.2020.11.2.05
[64] Lavezzo, E., Franchin, E., Ciavarella, C., Cuomo-Dannenburg, G., Barzon, L., Del Vecchio, C., ... & Abate, D. (2020). Suppression of COVID-19 outbreak in the municipality of Vo, Italy. medRxiv.https://www.medrxiv.org/content/10.1101/2020.04.17.20053157v1
[65] Mannheim, J., Gretsch, S., Layden, J. E., & Fricchione, M. J. (2020). Characteristics of Hospitalized Pediatric COVID-19 Cases—Chicago, Illinois, March–April 2020. Journal of the Pediatric Infectious Diseases Society. Available at https://academic.oup.com/jpids/advance-article/doi/10.1093/jpids/piaa070/5849922
[66] https://www.mass.gov/info-details/covid-19-response-reporting
[67] Wei Li, Bo Zhang, Jianhua Lu, Shihua Liu, Zhiqiang Chang, Cao Peng, Xinghua Liu, Peng Zhang, Yan Ling, Kaixiong Tao, Jianying Chen, Characteristics of Household Transmission of COVID-19, Clinical Infectious Diseases, , ciaa450, https://doi.org/10.1093/cid/ciaa450
[68] Jing, Q. L., Liu, M. J., Yuan, J., Zhang, Z. B., Zhang, A. R., Dean, N. E., ... & Lu, Y. (2020). Household secondary attack rate of COVID-19 and associated determinants. medRxiv. Available at https://www.medrxiv.org/content/10.1101/2020.04.11.20056010v1
[69] Mizumoto, K., Omori, R., & Nishiura, H. Age specificity of cases and attack rate of novel coronavirus disease (COVID-19). medRxiv 2020. Available at https://www.medrxiv.org/content/10.1101/2020.03.09.20033142v1
[70] Eli S Rosenberg, Elizabeth M Dufort, Debra S Blog, …, New York State Coronavirus 2019 Response Team, COVID-19 Testing, Epidemic Features, Hospital Outcomes, and Household Prevalence, New York State—March 2020, Clinical Infectious Diseases, https://doi.org/10.1093/cid/ciaa549
[71] Viner, R. M., Mytton, O. T., Bonell, C., Melendez-Torres, G. J., Ward, J. L., Hudson, L., ... & Panovska-Griffiths, J. (2020). Susceptibility to and transmission of COVID-19 amongst children and adolescents compared with adults: a systematic review and meta-analysis. medRxiv. Available at https://www.medrxiv.org/content/10.1101/2020.05.20.20108126v1
[72] Somekh, E., Gleyzer, A., Heller, E., Lopian, M., Kashani-Ligumski, L., Czeiger, S., ... & Stein, M. (2020). The Role of Children in the Dynamics of Intra Family Coronavirus 2019 Spread in Densely Populated Area. The Pediatric Infectious Disease Journal. Available at https://journals.lww.com/pidj/Abstract/9000/The_Role_of_Children_in_the_Dynamics_of_Intra.96128.aspx
[73] Zhu, Y., Bloxham, C. J., Hulme, K. D., Sinclair, J. E., Tong, Z. W. M., Steele, L. E., ... & Gilks, C. (2020). Children are unlikely to have been the primary source of household SARS-CoV-2 infections. Available at https://www.medrxiv.org/content/10.1101/2020.03.26.20044826v1
[74] Jing, Q. L., Liu, M. J., Yuan, J., Zhang, Z. B., Zhang, A. R., Dean, N. E., ... & Lu, Y. (2020). Household secondary attack rate of COVID-19 and associated determinants. medRxiv. Available at https://www.medrxiv.org/content/10.1101/2020.04.11.20056010v1
[75] Posfay Barbe, C., Wagner, N., Gauthey, M., Moussaoui, D., Loevy, N., Diana, A., & L'Huillier, A. (2020). COVID-19 in Children and the Dynamics of Infection in Families. Pediatrics, e20201576. Available at https://pediatrics.aappublications.org/content/early/2020/05/22/peds.2020-1576
[76] Mannheim, J., Gretsch, S., Layden, J. E., & Fricchione, M. J. (2020). Characteristics of Hospitalized Pediatric COVID-19 Cases—Chicago, Illinois, March–April 2020. Journal of the Pediatric Infectious Diseases Society. Available at https://academic.oup.com/jpids/advance-article/doi/10.1093/jpids/piaa070/5849922
[77] CDC, Considerations for Schools. (2020, May 19). Available at https://www.cdc.gov/coronavirus/2019-ncov/community/schools-childcare/schools.html
ref[78] How Denmark got its children back to school so soon after lockdown (2020, May 28). Available at https://www.thelocal.com/20200528/how-denmark-got-its-children-back-to-school
[79] CDC, Cleaning and Disinfecting Your Facility. (2020, April 14). Available at https://www.cdc.gov/coronavirus/2019-ncov/community/disinfecting-building-facility.html
[80] CDC, How To Clean and Disinfect Schools To Help Slow the Spread of Flu. (2018, July 31). Available at https://www.cdc.gov/flu/school/cleaning.htm
[81] CDC, Considerations for Schools. (2020, May 19). Available at https://www.cdc.gov/coronavirus/2019-ncov/community/schools-childcare/schools.html
[82] California Department of Education, Stronger Together
A Guidebook for the Safe Reopening of California's Public Schools. (2020, June 8). Available at https://www.cde.ca.gov/ls/he/hn/documents/strongertogether.pdf.
[83] Morawska, Lidia, et al. "How can airborne transmission of COVID-19 indoors be minimised?." Environment International (2020): 105832.
[84] CDC, Considerations for Schools. (2020, May 19). Available at https://www.cdc.gov/coronavirus/2019-ncov/community/schools-childcare/schools.html

